
Strong Nations Are Healthy and Inclusive
The mounting crises of the past year have challenged social, environmental and health systems. Large swathes of humanity have been left vulnerable to war, disease, and natural disasters, pushing millions closer to poverty. Many societies, even those in high-income and well-governed nations, are suffering from increased polarisation, entrenched inequality, and growing disunity.
These challenges do not appear to be abating. To build stronger and more resilient nations that are ready to confront the shockwaves of the ongoing polycrisis, governments will need to ensure that nobody is left behind. A recent study by the Oxford COVID-19 government response tracker found that it was not pandemic preparedness that correlated with fewer pandemic deaths, but levels of interpersonal trust
in society.1 It also found that societies with higher levels of interpersonal trust did not require very harsh lockdown measures as people could trust each other to follow social distancing guidelines.
These insights are key to understanding what governments can do to promote greater social cohesion and increase trust during a crisis. Tackling inequality, closing the gender gap, ensuring universal access to quality healthcare, and using education to enable social mobility are critical areas that governments can address to create more inclusive societies that engender trust. Ultimately, community and business actors need to work in unity with governments to prepare for the growing number of crises ahead.
The costs of inequality in societies have been well-documented. Experts estimate a cost of USD 22.9 trillion to the economy due to inequality in employment, education, and income over the past 30 years just in the US alone.2 The pandemic exposed the huge social and economic costs of years of under-investment in social protections such as healthcare. In Asia-Pacific alone, 60% of people have no access to social protection and 40% have no access to healthcare. These vulnerabilities from the lack of inclusive growth continue to hinder post-pandemic recovery.
Take the gender gap for example. Two years after the pandemic, the Global Gender Gap Report estimates that it will take 132 years to close the gender gap, and if not addressed could shrink the global economy by trillions of dollars by 2030.3 More gender-equal policies such as better maternity leave can help societies accelerate recovery. The IMF estimates that if women’s participation is on par with men’s, the global GDP would be 20% higher.4
Some governments have been better at prioritising inclusive growth when planning for the future, even when faced with limited tools, resources, and capital. This year, the Chandler Good Government Index (CGGI) has captured this with a number of countries making noted improvements in scores and rankings under Pillar 7: Helping People Rise. To find out how these governments have made inroads in creating better and more inclusive national outcomes despite facing a polycrisis, we asked ourselves the following questions: What makes these countries stand apart? What capabilities do these governments have? What policies and practices help mitigate crises to improve outcomes for all members of society? What can governments do to build healthy and inclusive communities that can confront the growing crises of our time?
Several countries, including Indonesia, Kenya, Portugal, Senegal and Costa Rica, were more successful in creating good national outcomes over the past year despite the polycrisis. These countries have maintained an integrative approach to post-pandemic recovery. A focus on green growth and sustainable policies, and the assurance that the vulnerable have larger social safety nets were some of the major factors of their success.
These countries and many others have learned to overcome limited resources to deal with short-term crises and generate long-term impacts. An ability to deal with short-term crises like the pandemic,
while investing in change that pays dividends in the future—such as closing gender gaps and promoting social inclusion—is key to society’s well-being and prosperity. To meet escalating global crises, the World Bank emphasised sustainability and inclusive growth, matched by trillions in investments in global public goods, as a priority for the global community.5
Instead of looking at health or social issues in policy siloes, governments that placed inclusive growth at the centre of development have been more successful at dealing with current shocks and planning for the future. For example, Indonesia’s capacity to shift budgets and policies to ensure inclusive growth remains a top-most priority to its government.
The pandemic has exacerbated inequalities and weaknesses in health and education systems throughout the globe. Some countries have invested heavily in health and education outcomes in response to these fault lines, while also thinking ahead of the impending climate crisis. We see this in Senegal’s and Costa Rica’s efforts to continue their impressive response to pandemic healthcare and improve primary healthcare. Other countries have focused on green growth and sustainable policies that ensure larger social safety nets for the vulnerable. Portugal’s innovative social inclusion policies are one great example.
Kenya’s efforts at decentralisation are an example of how nations have also used innovative systems of governance to promote inclusive development plans. Ultimately these country examples demonstrate that regardless of income level, size or resources, governments are exploring multiple policy levers to help people rise in response to the polycrisis.
Indonesia
Keeping Inclusive Growth a Central Priority
Indonesia’s experience with post-pandemic planning and recovery holds important lessons for peer countries on how to prioritise and promote inclusive growth by responding flexibly and changing policy priorities as needs shift. At the start of the pandemic in 2020, Indonesia launched a comprehensive budget known as the COVID-19 Handling and National Economic Recovery Programme (PC-PEN). In the first year of the programme, the focus was on boosting the healthcare sector, primarily in the procurement of vaccines and in social protections for vulnerable households. The budget also included support for SMEs and regional governments. As the pandemic wore on and new crises such as the increasing cost-of-living and inflation emerged, the government reallocated funds where it was most necessary, with healthcare and social protection programmes receiving the lion’s share of resources.6
Inclusive growth has been central to Indonesia’s policy directions and programmes, especially in the reforms to its healthcare system to close the gaps exposed by the pandemic. These gaps were primarily in uneven and unequal access to healthcare, inefficiencies in referral services, primary healthcare services, and unsustainable financing models. Learning from Indonesia’s experience of taking advantage of the 1998 Asian financial crisis to carry out large-scale transformations, President Jokowi announced a major health sector transformation blueprint in 2021 during the thick of the pandemic, and allocated 9.4% of the nation’s total budget to the programme.7
One of Indonesia’s major goals is to move toward more health promotion and prevention activities within its primary healthcare model. Integrated health services posts (Posyandu) and community health centres (Puskesmas) carry the bulk of primary healthcare in the nation. The Ministry of Health of Indonesia aims to standardise and expand the health services offered at health services posts to include lab testing and screening of chronic and endemic illnesses such as cancer and tuberculosis.8 City hospitals will also be better equipped to conduct moderate-level surgical operations such as heart stents, and provincial hospitals will be upgraded and enabled to offer all major medical procedures. These developments go a long way toward promoting equitable health access in Indonesia. The Indonesian health sector learned the importance of digitisation in modernising and streamlining healthcare during the pandemic. In response, the Indonesian government has already started rolling out a big-data record-keeping system for all government hospitals.

To close the inequality gap, President Jokowi set out to reduce the Gini coefficient to the range of 0.376-0.378 in 2022 through a range of social protection schemes. The government identified 161 million poor and vulnerable people that would receive assistance to meet basic needs such as housing, food, energy bills and education. The education sector was also uplifted by cash provisions to students from low-income families to increase enrolment rates.9 COVID-19 exposed the problem of inequity in education—girls, the poor, children with disabilities, and those speaking minor languages were disproportionately affected by school closures. This has prompted more investment in supporting vulnerable students’ access to quality education. For example, reforming the curriculum in the early years to focus more on literacy and numeracy rather than traditional subjects, promotes better learning outcomes for vulnerable groups. National exams which are high-stakes and often privilege students from wealthier backgrounds were also scrapped during the pandemic as testing was not possible. This prompted a move towards competency-based assessment models.10
These comprehensive social protection, health, and education schemes that Indonesia adopted this past year are reflected in Indonesia’s 2023 rankings for the CGGI’s Helping People Rise pillar, which moved up five places to rank 68th.
Kenya
Inclusivity and Responsiveness Through Decentralisation
Among the 2010 constitutional reforms in Kenya was a rethinking of governance structures that, in the words of former President Uhuru Kenyatta, left an “impactful and transformative” result.11 A significant element of the reforms was the transfer of decision-making authority, or devolution, for a variety of policy domains, ranging from local health to commerce, from the central government to county governments. In an effort to reduce regional inequality and give communities a greater say over their own affairs, the reform also aimed to “give powers of self-governance to the people”.
Since the implementation of devolution across Kenya’s 47 counties in 2013, notable advances have been made towards increasing participation of the public, reducing unnecessary bureaucracy, fostering local economic growth and contributing to a more equitable distribution of natural resources.12 13 14 Of all the notable benefits, those related to “Helping People Rise” provide potent lessons for policymakers who recognise that enhancing the welfare of the citizenry goes hand in hand with economic development.15 One of the most practical ways that this devolution has promoted inclusivity, particularly for women and minorities, has been with participatory budgeting.

The process ensures that public funds are used to meet citizens’ needs and that citizens have greater oversight over how money is spent. While there are still many challenges in getting more participation from youth, women and minorities in this process, a focus on participatory budgeting has opened up spaces for regional governments to think about how to raise capacity for increased public participation, and to get more people to the decision-making table.
Devolution is also bringing tangible benefits for Kenya as the nation builds on its infrastructure of social resilience to mitigate crises. Although there are challenges to adjusting to a decentralised health sector, the process enabled greater opportunities for populations to participate in the creation of governance systems for healthcare. It also gave more responsibility to local-level leaders, who are naturally closer to their constituents.16 17 Overall, there was a marked improvement in the structure of healthcare provision.18 In some local counties, health sector stakeholders, such as health workers, were also able to actively participate in the design of local healthcare offerings.19
Budgeting in Kenya has also benefitted from devolution. All areas of government financing from healthcare to infrastructure have undergone revisions. Giving space to local government actors to determine the most appropriate use of funds enables policymaking to be closer to the ground. The notion of participatory budgeting also became possible in an effort to enable local stakeholders to contribute to budgeting processes. In some counties in Kenya, this influenced how much public funds were spent on the needs of the citizenry and provided oversight of public expenditures.20 While the full impact of devolution in the country continues to be analysed by academics and bureaucrats, the process has empowered local authorities to make policies that are closer to the ground realities of the people they ultimately serve. Kenya’s ranking in this year’s CGGI in the Helping People Rise pillar rose nine places to 84th, and notably rose 21 spots in the Satisfaction with Public Services indicator to 61st.
Portugal
A Long-Standing Commitment to Inclusion and Equality
Portugal moved up three places this year in the Helping People Rise pillar and ranks 21st. One of the most forward-thinking aspects of Portugal’s inclusive policymaking this past year has been the emphasis on health, housing, and education. A key hallmark of its 2021 recovery and resilience plan was its strong social protection measures. Portugal was badly affected by the 2008 financial crisis and adopted a series of austerity measures through the early 2010s by cutting back public spending on social inclusion and programmes aimed at targeting poverty. This led to roughly a 2% increase in the share of those at risk of poverty between 2010 and 2015. Even before the pandemic, Portugal recognised the detrimental effects of long-term austerity on social inclusion. The nation boosted welfare and pension funds, resulting in a fall from 19.5 % in 2015 to 16.2% in 2020 for those at risk of poverty after social transfers even during the pandemic.21
Building on these modest gains in poverty reduction, the 2021 plan prioritises investments in the National Health Service. During the second wave of COVID-19, Portugal’s health system was severely strained. Its government responded with major financial investment in the health sector to fill labour gaps by increasing the number of doctors and nurses. One of the main lessons gained by Portugal during the pandemic is the importance of ensuring that the most vulnerable groups can continue to access healthcare. This was supported by an increase in telehealth medicine. Arguably, the longer-term investment by the Portuguese government in poverty reduction and social inclusion helped to build trust, which also resulted in high rates of vaccination. The 2021 plan also has investments aimed at strengthening the National Health Service, which provides universal healthcare, and extending the coverage of social services—this includes long-term care and measures to support people with disabilities.22

As early as 2020, the government also introduced inclusive family policies aimed at alleviating labour burdens on women. Paternity leave was extended from 15 to 20 days. Families with children under the age of three now enjoy tax deductions and financial support for early-childhood education. Low-income families are able to freely access pre-kindergarten services.
Two innovative policies in Portugal stand out in promoting social inclusion at local levels. The 2021 plan pledged EUR 250 million to support social interventions in poor urban areas and an innovative social housing programme. Access to decent living environments and quality buildings for housing helps to build resilience not only in social terms, but also in practical terms as the recent earthquakes in Türkiye and Syria have demonstrated. The social housing investment, worth EUR 1.2 billion, is being rolled out across Portugal. Investments in housing needs within a locality are coordinated between the national and municipal governments. At least 26,000 households will benefit from decent and adequate housing by 2026, including families that require financial assistance and groups that are vulnerable. The scheme includes the construction of new buildings or the renovation of existing homes and buildings, as well as the acquiring or leasing of new buildings where necessary.23
Portugal’s approach to inclusive education attempts to tackle the relatively low secondary and tertiary completion rates for a high-income country. As the country moves to a more green and digital economy, matching educational programmes with in-demand skills is key to ensuring access to the formal labour market. Thus the education reform includes the modernisation of vocational education institutions to better match skills development to the needs of the market, and the boosting of skill levels of the population, allowing more young people to access employment.
Through Europe’s ongoing migration crisis, Portugal has always maintained inclusive and open policies for refugees, naturalisation and integration. Portugal is a global leader in inclusive social policies for new arrivals, most notably granting citizenship to children of undocumented migrants after a year of arrival, and all children regardless of legal status can access education. All immigrants, even undocumented ones, can raise complaints to the Commission on Equality for Racial Discrimination.
Overall, with a focus on social inclusion across sectors, such as a stronger safety net for the poor, greater access to quality healthcare, housing and education as well as an upskilled workforce, Portugal seems poised to contend successfully with complex crises.
Senegal
Looking to the Past to Prepare for the Future: Building More Resilient Health Systems
Sub-Saharan African countries that handled Ebola were well-placed to deal with COVID-19. Drawing on lessons from Ebola, these countries are shoring up their health systems to face future shocks despite limited resources. One such country is Senegal, which moved up three places from 86th to 83rd in this year’s Health indicator under the Helping People Rise pillar.
Senegal established its Health Emergency Operations System in 2014 in response to the Ebola outbreak; the system was designed to be a permanent emergency response system. This early investment proved critical in the country’s relatively successful COVID-19 response. As the pandemic began, the government unit was able to quickly establish a regime of rapid testing, isolation and treatment of cases. Senegal also relied on its strong research capacity to facilitate rapid testing. At the start of the pandemic, the Pasteur Institute in Dakar was the only facility able to test for COVID-19, but within months, field labs had been established in all its regions and 48-hour testing has become the gold standard.24
Health systems in nations with large rural areas are not always accessible. Decentralisation and a reliance on community health clinics have proved essential to Senegal in ensuring basic healthcare access. Local teams were mobilised to curb the spread of COVID-19. The Senegalese government saw the need to move quickly to increase isolation and treatment capacity, and thus rapidly trained personnel to set up field hospitals and treat patients. This national approach was replicated in all regions. Senegal has 14 medical regions, further subdivided into 79 health districts. The districts have health centres with doctors and nurses, and a further subdivision of postes de santé, or health posts staffed by a nurse or midwife. These community health workers became essential nodes in building trust in the community and educating them about COVID-19. The capacity to coordinate between state and local government, right down to the health clinic level, was a critical part of ensuring universal support to all citizens in handling the virus.
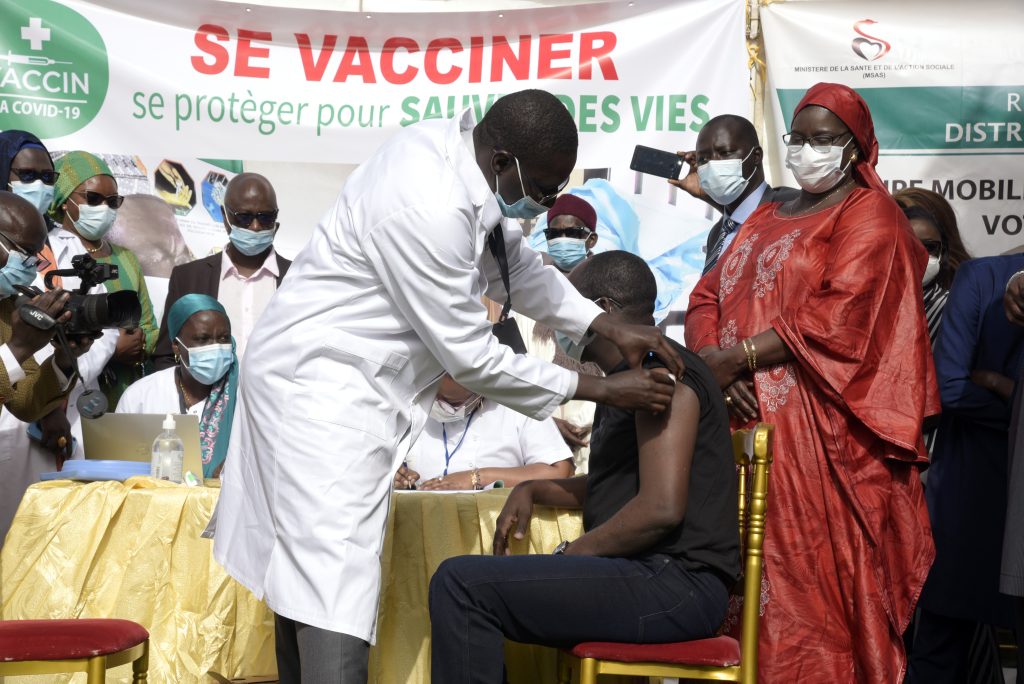
Even more impressively, while creating a comprehensive national approach to COVID-19, Senegal worked hard to ensure the continuity of essential health services. This was made possible with its nimble subnational public health model that allowed information and services to flow freely between the capital to all areas of the country. Community health centres were mapped, ensuring that reproductive, maternal and child health services could still be provided. The government supported private clinics to continue their primary care functions and paid for any COVID-19 treatments. During lockdowns, the government also adapted its ongoing disease management programmes, such as home delivery of antiretroviral and tuberculosis drugs so patients could avoid going to health centres. Community health workers also relied on phone and video calls to continue patient management and support.25
Post pandemic, Senegal has increased funding for all entities and bodies working to respond to acute outbreaks. The nation has continued to invest in its community health centres and build local capacity to close gaps in the provision of basic healthcare. The Senegalese government has also launched programmes to support the most vulnerable members of the community: women, youth, children and people with disabilities. A three-year emergency programme was started to promote youth employment and socio-economic inclusion. During the pandemic, the government quickly reallocated its budget to invest in priority sectors, such as healthcare and social support programmes for the most vulnerable, particularly those living with disabilities, and this has continued after the pandemic. These social support programmes include food distribution, and the payment of utility bills.26
While Senegal works to close gaps in basic healthcare provisions and access in rural areas, the government has capitalised on the lessons from the pandemic to promote digitisation. Prior to the pandemic, the government launched a comprehensive digitisation of the health sector roadmap as part of its efforts to streamline the country’s health system coverage. This included the use of telemedicine, helping hospitals to digitise health records and promoting biomedical innovation. The pandemic saw the launch of a digital health certificate, known as the SMART health card, aimed primarily at updating vaccination status and test results. The e-health card has since transitioned into providing up-to-date health information for its users.27
These lessons from Senegal’s COVID-19 response and post-COVID investments are important as they demonstrate that even with fewer resources, governments that prioritise inclusive health policies are better prepared for new health crises on the horizon.
Costa Rica
Responding Comprehensively to the Pandemic to Bolster Healthcare and Social Protections
Costa Rica’s approach to a healthy nation highlights the importance of long-term investments in healthcare and education. These investments prepared Costa Rica to face the crisis of the pandemic and the shockwaves of the evolving polycrisis that lie ahead. In this year’s index, Costa Rica moved up five places to rank 48th in the Helping People Rise pillar.
From as early as the 1940s when Costa Rica dismantled the coffee oligarchy and military, government spending has focused on creating social safety nets, robust public health and education access—all of which are key factors in ensuring resilient systems that support all citizens. Costa Rica is the only country in Central America where everyone has access to electricity and clean drinking water, and one of the few in the region to offer universal healthcare.28
By the 1970s, Costa Rica was spending more on health as a proportion of GDP than many high-income countries. The public health system also relied on a community health model that brought health access to local communities. Local teams of doctors, nurses, and community health workers would visit households annually to assess their needs. This allowed Costa Rica to have a comprehensive picture of the health needs, and the social and environmental conditions affecting the health and well-being of almost all of its residents. The country had also contended with public health outbreaks and natural disasters in the past and had installed emergency preparedness measures. These historic developments helped Costa Rica to swiftly respond to COVID-19.
Costa Rica’s response to the pandemic also benefitted from a centralised government that coordinated across all ministries, and the close partnerships it enjoys with the private sector and universities. The government was also able to capitalise on the strong social and community bonds in the country to mount a united response to the pandemic.
Some of the hallmarks of Costa Rica’s comprehensive national pandemic strategy included coordination across government agencies, localised responses, effective communication with the public, reliable information and data flows that helped informed policy, financial assistance, and support to business and tourism sectors. Costa Rica also recognised that this was not just a health crisis, but also a social one. Its policy responses always reflected a careful balancing act between health and economic needs. Costa Rica never adopted a full lockdown like many countries in Latin America, and instead focused on stricter lockdowns in hotspots and more relaxed measures in regions with a low number of cases.29 In November 2020, Costa Rica was the first country in Latin America to open its borders to tourists and even dropped testing requirements for visitors.30 As the pandemic wore on, Costa Rica continued to draw on the principles of coordinated government response, strong public and private partnerships, sound decision making that balanced acute needs with long-term effects, and effective localised containment measures.
Despite these efforts, Costa Rica still saw a 26% rise in households falling into poverty and a rise in income inequality. This was largely due to systemic issues brewing over the past decade which include low access to opportunities for lesser-educated workers, an ageing population and strikingly low labour participation of women compared to neighbouring countries.31 32
Moving forward, the Costa Rican government has continued to look broadly at the challenges that lie ahead as it prioritises its investments. Even during the pandemic, health authorities were already reviewing and revising emergency preparedness guidelines and protocols in preparation for a new pandemic. Another important step the government has taken is to look at future challenges in holistic and integrated ways to identify policy objectives accordingly. Its pandemic recovery plans focus on how to support society’s most vulnerable members, ensure the sustainability of public finances and champion low-carbon green growth. Some initiatives include the use of cash transfers to the poorest, measures to help small-medium enterprises (SMEs) and preserve jobs, the increase of tax revenue and acceleration of deployment of green technologies. Costa Rica looks well-positioned to dismantle inequalities and steel itself against upcoming crises.

Endnotes
- Hale, T. (2022, March 24). We’ve found one factor that predicts which countries Best Survive covid | Thomas Hale. The Guardian. Retrieved March 9, 2023, from https://www. theguardian.com/commentisfree/2022/mar/24/countries-covid-trust-damage-pandemic
- Buckman, S. R., Choi, L. Y., Daly, M. C., Seitelman, L. M. (2022, August 23). The economic gains from equity. Brookings. Retrieved March 9, 2023, from https://www.brookings.edu/bpea-articles/the-economic-gains-from-equity/
- Sawhney, I. (2023, January 13). 3 ways to reduce gender inequality in the workplace post COVID-19. World Economic Forum. Retrieved March 9, 2023, from https://www. weforum.org/agenda/2023/01/gender-equality-covid-19-workplace-davos23/
- Georgieva, K. (2023, March). IMF Chief to CNN: “Gender Equality is Good Economics”. Retrieved March 20, 2023, from https://www.linkedin.com/posts/kristalina-georgieva_iwd-activity-7039385381422657536-3H1w
- The World Bank. (2022, October 21). Inclusive growth: The key to a lasting recovery. World Bank Live. Retrieved March 9, 2023, from https://live.worldbank.org/events/annual-meetings-2022-inclusive-growth
- Jokowi introduces expansive 2022 budget bill, promises reform to overcome prolonged pandemic, uneven global recovery. Jakarta Globe. (2021, August 17). Retrieved March 9, 2023, from https://jakartaglobe.id/business/jokowi-introduces-expansive-2022-budget-bill-promises-reform-to-overcome-prolonged-pandemic-uneven-global-recovery
- Suhenda, D. (2023, January 9). Indonesia seeks post-pandemic healthcare system reform. Asia News Network. Retrieved March 9, 2023, from https://asianews.network/indonesia-seeks-post-pandemic-healthcare-system-reform/
- Ibid.
- Budianto, V. (2022, September 13). How social protection can create a more equal Indonesia. Asia & The Pacific Society
- Policy Forum. Retrieved March 9, 2023, from https://www. policyforum.net/how-social-protection-can-create-a-more-equal-indonesia/
- Heyward, M. (2022, May 24). Covid-19 and education reform in Indonesia. Devpolicy Blog from the Development Policy Centre. Retrieved March 9, 2023, from https://devpolicy.org/covid-19-and-education-reform-in-indonesia-20220525/
- The seventh and final annual Devolution Conference on Multi-Level Governance for Climate Change: United Nations Development Programme. UNDP Kenya. (2021, December 6). Retrieved March 9, 2023, from https://www.undp.
org/kenya/blog/seventh-and-final-annual-devolution-conference-multi-level-governance-climate-change - PricewaterhouseCoopers. (n.d.). Devolution: Are we making progress? – PWC. PwC Insight and Analysis. Retrieved March 9, 2023, from https://www.pwc.com/ke/en/assets/pdf/devolved-function.pdf
- World Bank Group. (2015, February 4). Kenya: Devolution and infrastructure boost growth and shared prosperity. The World Bank. Retrieved March 9, 2023, from https://www.worldbank. org/en/news/press-release/2015/02/04/kenya-devolution-and-infrastructure-boost-growth-and-shared-prosperity
- Ngigi, S., & Busolo, D. N. (2019). Devolution in Kenya: The Good, the Bad and the Ugly. Public Policy and Administration Research, 9(6). https://doi.org/10.7176/ppar
- Boosting Accountability through Participatory Budgeting in Kenya. (n.d.). In Enhancing Government Effectiveness and Transparency: The Fight Against Corruption. essay. Retrieved March 9, 2023, from https://thedocs.worldbank.org/en/ doc/571511611672507228-0090022021/original/Boosting AccountabilitythroughParticipatoryBudgetinginKenya.pdf.
- Muwonge, A., Williamson, T. S., Owuor, C., & Kinuthia, M.(n.d.). Making Devolution Work for Service Delivery in Kenya. Retrieved March 9, 2023, from https://openknowledge. worldbank.org/server/api/core/bitstreams/1f6f28b6-72b1-5498-a77a-d0d4a205151c/content.
- McCollum, R., Limato, R., Otiso, L., Theobald, S., & Taegtmeyer, M. (2018). Health system governance following devolution: Comparing experiences of decentralisation in Kenya and Indonesia. BMJ Global Health, 3(5). https://doi. org/10.1136/bmjgh-2018-000939
- Masaba, B. B., Moturi, J. K., Taiswa, J., & Mmusi-Phetoe,
R. M. (2020). Devolution of healthcare system in Kenya: Progress and challenges. Public Health, 189, 135–140. https://doi.org/10.1016/j.puhe.2020.10.001 - Lipsky, A., Mulaki, A., Williamson, T., & Sullivan, Z.
(2015). (rep.). Political Will for Health System Devolution in Kenya: Insights from Three Counties. Health Policy Project. Retrieved March 9, 2023, from https://www.healthpolicy project.com/pubs/511_KenyaPoliticalWillbrief.pdf. - Boosting Accountability through Participatory Budgeting in Kenya. (n.d.). In Enhancing Government Effectiveness and Transparency: The Fight Against Corruption. essay. Retrieved March 9, 2023, from https://thedocs.worldbank.org/en/doc/571511611672507228-0090022021/original/Boosting AccountabilitythroughParticipatoryBudgetinginKenya.pdf
- BertelsmannStiftung. (n.d.). SGI Sustainable Governance Indicators 2020: Portugal. SGI 2020 | Portugal | Social Policies. Retrieved April 11, 2023, from https://www.sgi-network.org/2020/Portugal/Social_Policies
- Portugal: Country Health Profile 2021. (2021). State of Health in the EU. https://doi.org/10.1787/8f3b0171-en European Commission. (n.d.). Portugal’s recovery and resilience plan. European Commission. Retrieved March
9, 2023, from https://commission.europa.eu/business-economy-euro/economic-recovery/recovery-and-resilience-facility/portugals-recovery-and-resilience-plan_en - Kirby, J. (2021, April 28). How Senegal stretched its health care system to stop Covid-19. Vox. Retrieved March 9, 2023, from https://www.vox.com/22397842/senegal-covid-19-pandemic-playbook
- Kabwama, S. N. et al. (n.d.). Essential Health Services: Senegal. Senegal | Exemplars in Global Health. Retrieved March 9, 2023, from https://www.exemplars.health/emerging-topics/epidemic-preparedness-and-response/essential-health-services/senegal
- International Budget Partnership. (2021). (rep.). Transparency and Credibility of COVID Response in Senegal. Retrieved March 9, 2023, from https://internationalbudget.org/covid/wp-content/uploads/2021/08/Senegal-Brief-Managing-COVID-Funds.pdf.
- Toure, A., & Mbengue, B. (2022, December 12). 100,000 Reasons to Celebrate: Senegal Reaches Important Milestone on the Road to Digitalisation. Retrieved March 9, 2023, from https://www.institute.global/insights/public-services/100000-reasons-celebrate-senegal-reaches-important-milestone-road-digitalisation
- Bala, A. (2022, March 9). Costa Rica Prioritizes Public Health. IMF News: IMF Country Focus. Retrieved March 9, 2023, from https://www.imf.org/en/News/Articles/2022/03/09/cf-costa-rica-prioritizes-public-health
- ibid
- Reports, S. (2021, September 16). The hidden impact of covid-19 on poverty in Costa Rica. BORGEN Magazine. Retrieved March 9, 2023, from https://www.borgen magazine.com/impact-of-covid-19-on-poverty-in-costa-rica/
- Verde, M. (2022). (rep.). Global Challenges COVID-19: Innovations for Successful Societies. The Value of Vigilance: Costa Rica’s First-Year Response to COVID-19, 2020. Retrieved March 11, 2023, from https://successfulsocieties. princeton.edu/sites/ successfulsocieties/files/Costa%20 Rica_COVID_Final_0.pdf
- Hoop, J. D., & Arakaki, A. (2022, September 27). Why are poverty and inequality not declining in Costa Rica?World Bank Blogs. Retrieved March 9, 2023, from https://blogs.worldbank.org/latinamerica/why-are-poverty-and-inequality-not-declining-costa-rica
More Stories


Regional Insights: Latin America & Caribbean

